Broiler meat, main food implicated in Campylobacter food-borne infections
The latest zoonoses report published by EFSA for 2021 confirms that campylobacteriosis is the most reported food-borne gastrointestinal infection in the EU. This has been the case since 2007.
The number of confirmed cases of campylobacteriosis was 127,840, or 41.1 cases per 100,000 population. Broiler chicken caused the highest number of outbreaks detected in the EU, with a total of 7 outbreaks, followed by mixed foods (5 outbreaks), beef and beef-based products (3 outbreaks) and finally other poultry meat, mixed or unspecified, and poultry products.

Figure 1. Reported numbers of cases and notification rates for confirmed human zoonoses in the EU, 2021
In the table below, it can be seen how the occurrence and prevalence of Campylobacter in food and animals between 2017 and 2021, had a slight increase of reported human cases. Since 2019, the number of sampling units reported for “meat and meat products” has increased considerably, probably due to the Commission Implementing Regulation Commission Regulation (EU) 2019/627 establishing mandatory reporting of Campylobacter SDA monitoring data.

Table 1. Summary of Campylobacter, statics related to humans, major food categories and the main animal species, EU, 2017-2021.
As with other microorganisms there is a clear seasonality in the number of confirmed cases of campylobacteriosis in the EU/EEA, with peaks in the summer months. Annual winter peaks can also be seen in Figure 2 in the month of January 2112 to 2021 although these are lower than the numbers observed during the summer. In 2021, as was already the case in 2020, the number of cases decreased, probably due to the Covid-19 pandemic.

Figure 2. Trends in reported confirmed human cases of campylobacteriosis in the EU, by month, 2017–2021
The controls established by the EU showed positive percentages in RTE and non-RTE foodstuffs of 0.31% and 10.9%. Although the presence of Campylobacter in food for consumption is low, it is nevertheless worrying because this type of product directly exposes consumers to the disease. Regarding the data for non-RTD foods, positive results were found in 1 out of 10 in the category “meat and meat products” (table 2).
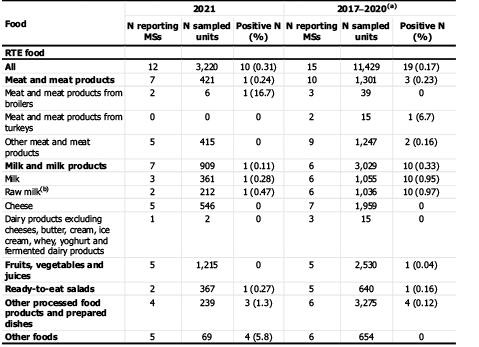
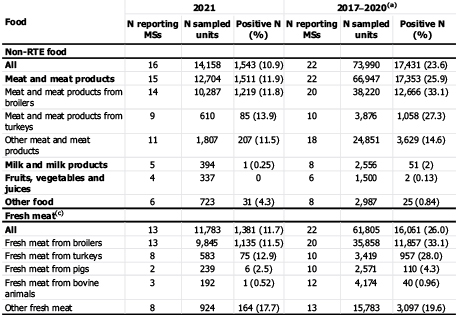
Table 2. Occurrence of Campylobacter in the main food categories, EU, 2021 and 2017-2020
What is Campylobacter?
Campylobacter is a genus of small, Gram-negative, non-sporulating bacteria, comprising different species, most notably C. jejuni and C. coli, which cause infections in humans. They are considered to be demanding bacteria, as they require reduced oxygen environments for growth and temperatures above 30 °C.
Campylobacter spp. are sensitive to desiccation, acidic pH and many disinfectants, yet they remain one of the main bacteria causing foodborne illness.

Table 3. Campylobacter, growth factors.
Reservoirs and transmission
The most common reservoir of Campylobacter is the intestinal tract of mammals and birds. Animals rarely develop the disease, but the bacteria can contaminate food obtained from them, such as milk and dairy products, meat and to a lesser extent, fresh vegetables and fishery products. Campylobacter is mainly found in poultry, due to their higher body temperature, and it is the consumption of chicken meat and processed chicken products that is the main source of campylobacteriosis cases in humans, constituting a public health problem with a significant social cost.
Water from rivers, lakes, seas, etc. can also be a frequent source of this micro-organism, mainly due to faecal contamination. Transmission to humans occurs mostly indirectly through consumption of contaminated food, but also through direct contact with domestic animals. In turn, humans can be a reservoir for this micro-organism. The different reservoirs and transmission routes are detailed in Figure 3.

Figure 3. Campylobacter reservoirs and transmission.
Campylobacter and biofilms
Campylobacter jejuni is capable of forming biofilms in vitro and on surfaces at different points in the poultry meat production chain. These biofilms can be found on farms, where the presence of C. jejuni biofilms in water pipes can play an important role in the colonisation of animals and on different surfaces in the slaughterhouse or cutting room.
C. jejuni is also found in biofilms of a mixed character, which are predominant in most environments, in these cases the bacterium acts as a secondary coloniser. The biofilm provides a number of advantages to C. jejuni as it facilitates the exchange of genetics, nutrients, enzymes, etc., so the biofilm poses a significant risk due to its ability to harbour pathogenic microorganisms and facilitate their survival.
Regulations and legal requirements
In 2010 EFSA published the analysis on the prevalence of Campylobacter in broiler flocks and carcasses. The study was carried out in 2008 in slaughterhouses and concluded that broiler carcasses were contaminated by an average of 75.8%, with significant variations between Member States and between slaughterhouses (EFSA 2010). EFSA’s 2010 scientific opinion on the risk of human campylobacteriosis related to broiler meat indicates that the handling, preparation and consumption of broiler meat is likely to account for 20-30% of the cases of human campylobacteriosis, while 50-80% is attributed to the chicken reservoir as a whole.
In view of the high incidence of Campylobacter in the population and the clear link with chicken meat consumption, an EFSA Scientific Opinion was published in 2011, estimating that setting a microbiological limit of 1,000 cfu/g could lead to a reduction of more than 50% of the public health risks from consumption of broiler meat (EFSA 2011). Consequently, in 2017, European Commission Regulation (EU) 2017/1495 amending Regulation (EC) 273/2005 as regards Campylobacter in broiler carcasses was published (European Commission 2017).
This regulation adapts the inspection methods for poultry carcasses with regard to Campylobacter and establishes a hygiene criterion for chicken carcasses, which aims to control the contamination of carcasses during the slaughter process. According to this criterion, in the Campylobacter count in broiler carcasses after chilling, no more than 40 % of samples exceeding 1,000 cfu/g should be accepted, from 2020 the percentage is reduced to 30 % and in 2025 to 20 %.
Strategies for the control of Campylobacter in the poultry sector
Control of Campylobacter in the poultry sector is of great strategic importance to avoid risk in humans. Control strategies should be implemented at all stages of the food chain, however, they will have the greatest impact at farm level, as the poultry intestine is the point in the chain where amplification of contamination occurs.
On farms, biosecurity is the most efficient strategy to reduce the prevalence of Campylobacter, consisting of the set of practices, procedures, behaviours, etc. that create barriers against infectious agents and prevent them from coming into contact with the animals. Three of the most important aspects of biosecurity are isolation and physical barriers, sanitisation and pest control. Cleaning and disinfection of broiler houses at the beginning of each production cycle is essential to reduce the risk of Campylobacter infection of broilers.
The concentration of Campylobacter in the faecal content is normally high, therefore, there is a dispersion of the microorganism to the materials and equipment with which the birds come into contact not only on the farm, but also during transport and slaughter at the slaughterhouse. In the slaughterhouse, carcasses can be contaminated at different stages of the processing chain, especially in the scalding-plucking, evisceration and cooling tanks. A number of strategies can be applied in the slaughterhouse and processing industries to complement those implemented at farm level, including scheduled slaughter, reduction of product contamination and hygiene of facilities and associated elements. The design of specific cleaning and disinfection procedures, focusing on critical points, are necessary to control contamination on the surfaces of the facility.
Bibliography
- EFSA (2022) The European Union One Health 2021 Zoonose Report. https:// doi/epdf/10.2903/j.efsa.2022.7666. https://efsa.onlinelibrary.wiley.com/doi/epdf/10.2903/j.efsa.2022.7666
- Orihuel, E., Bertó R., Canet J., Lorenzo F., Corujo A., Sanz M., Milvaques A., Canet JJ. (2015). Campylobacter, la bacteria discreta. Ed. Betelgeux, Gandia
- WHO– World Health Organization (2020). Campylobacter. https://www.who.int/es/news-room/fact-sheets/detail/campylobacter Consultado el 20/01/2021.
- Ryan J. Reeser, Robert T. Medler, Stephen J. Billington, B. Helen Jost, and Lynn A. Joens (2007). Characterization of Campylobacter jejuni Biofilms under Defined Growth Conditions. Appl Environ Microbiol, 73(6): 1908–1913.
- Roberta T. Melo, Eliane P. Mendonça, Guilherme P. Monteiro, Mariana C. Siqueira1, Clara B. Pereira1, Phelipe A. B. M. Peres, Heriberto Fernandez and Daise A. Rossi (2017). Intrinsic and Extrinsic Aspects on Campylobacter jejuni Frontiers in microbiology, Volume 8, Article 1332
- EFSA (2010). Scientific Opinion on Quantification of the risk posed by broiler meat to human campylobacteriosis in the EU. https://doi.org/10.2903/j.efsa.2010.1437
- EFSA (2011). Analysis of the baseline survey on the prevalence of Campylobacter in broiler batches and of Campylobacter and Salmonella o broiler carcasses in the EU, 2008 – Part A: Campylobacter and Salmonella prevalence estimates. https://doi.org/10.2903/j.efsa.2011.2017
- European Comission (2017). Reglamento (UE) 2017/1495 de la Comisión de 23 de agosto de 2017. https://eur-lex.europa.eu/legal-content/ES/TXT/PDF/?uri=CELEX:32017R1495&from=PL
- EFSA and ECDC (2019). The European Union One Health 2018 Zoonoses Report. https://doi.org/10.2903/j.efsa.2019.5926
EFSA (2020). Update and review of control options for Campylobacter in broilers at primary production https://doi.org/10.2903/j.efsa.2020.6090 - AESAN (2012). Informe del Comité Científico de la Agencia Española de Seguridad Alimentaria y Nutrición (AESAN) con relación a las medidas de control para reducir la presencia de Campylobacter en carne fresca de aves (pollo). AESAN-2012-005 https://www.aesan.gob.es/AECOSAN/docs/documentos/seguridad_alimentaria/evaluacion_riesgos/informes_comite/CAMPYLOBACTER.pdf
Authors

Team CHRISTEYNS Food Hygiene
Company specialized in food safety with headquarters Belgium. With more than 25 years of experience, we offer innovative and effective solutions to the specific hygiene problems of food factories, as well as livestock farms, through a wide range of products, equipment and services designed for the proper cleaning and disinfection of facilities.





